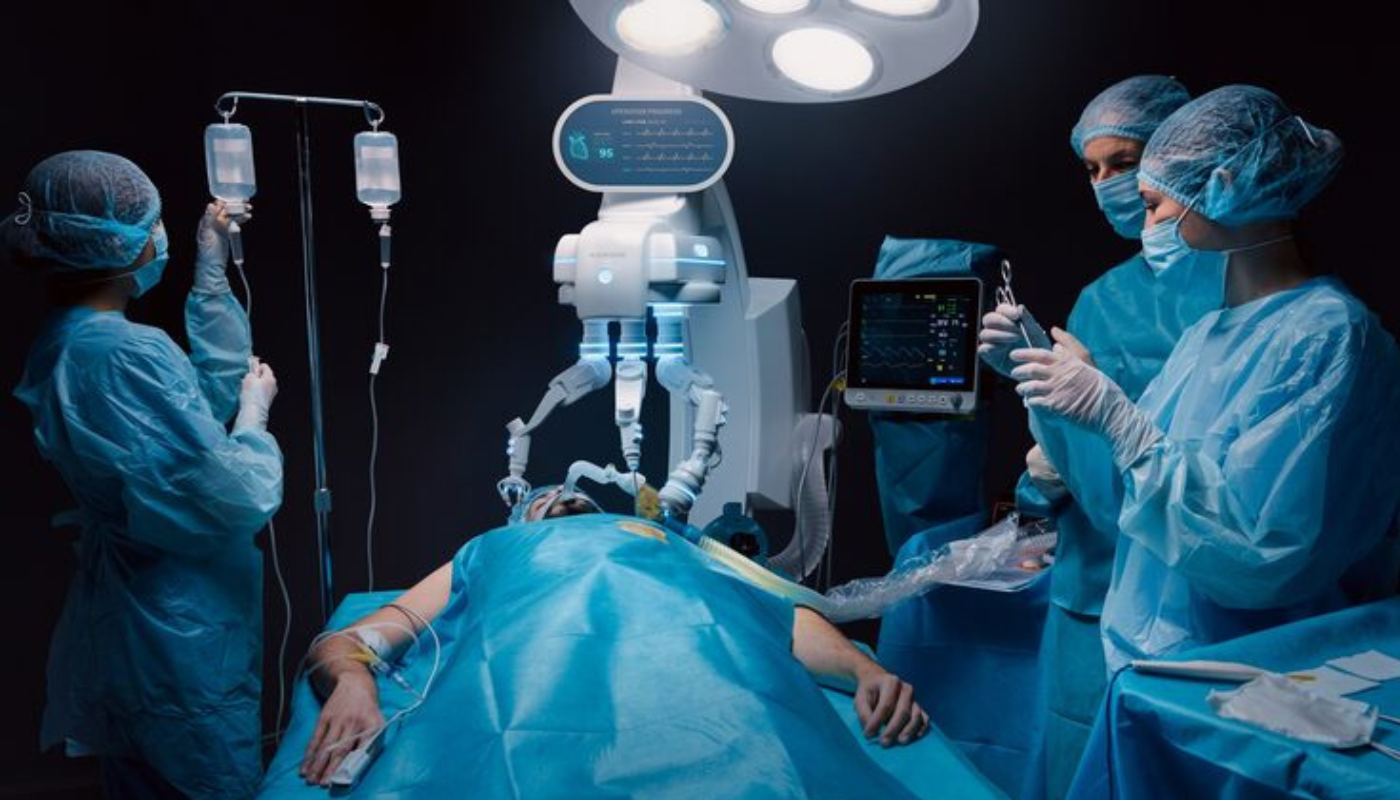
Robotic surgery in gynecology is an advanced and rapidly evolving form of minimally invasive surgery that utilizes sophisticated computer-assisted systems to aid surgeons in performing highly precise and complex procedures. This technology represents a significant leap forward from conventional surgical methods. In robotic-assisted surgery, the surgeon does not operate directly on the patient but instead controls robotic arms from a specialized console. These robotic arms are equipped with miniaturized surgical instruments that can mimic and even exceed the range of motion of the human hand, allowing for exceptional dexterity and control. The system also provides high-definition, three-dimensional visualization of the surgical field, enabling surgeons to view anatomical structures with remarkable clarity and depth. This enhanced visualization is especially valuable when operating on delicate tissues and confined spaces within the pelvic region.
Over the past decade, robotic surgery has significantly transformed the management of a wide range of gynecological conditions. It is now commonly used for procedures such as hysterectomy (removal of the uterus), myomectomy (removal of uterine fibroids), treatment of endometriosis, ovarian cyst removal, pelvic organ prolapse repair, and oncologic surgeries for cancers of the cervix, uterus, and ovaries. The precision offered by robotic systems allows surgeons to perform meticulous dissection and suturing, which is particularly beneficial in fertility-preserving procedures and complex cancer surgeries where preserving surrounding healthy tissue is crucial.
One of the most notable advantages of robotic surgery is its minimally invasive nature. Unlike traditional open surgery, which requires large incisions, robotic procedures are performed through very small incisions. This results in minimal scarring, reduced blood loss, lower risk of infection, and significantly less postoperative pain. As a result, patients often experience shorter hospital stays, quicker recovery times, and a faster return to normal daily activities. Additionally, the enhanced precision and stability of robotic instruments can lead to improved surgical outcomes and reduced complication rates.
Another key benefit is the ergonomic advantage for surgeons. Traditional laparoscopic surgery can be physically demanding due to awkward hand positions and limited instrument mobility. In contrast, robotic systems allow surgeons to operate in a comfortable seated position with intuitive controls, reducing fatigue and potentially improving performance during long and complex procedures. The elimination of natural hand tremors through robotic technology further enhances surgical accuracy.
Despite its many advantages, robotic surgery does have certain limitations. One of the primary challenges is the high cost associated with purchasing, maintaining, and operating robotic systems. This makes the procedures more expensive for healthcare providers and patients, limiting accessibility in many regions, particularly in smaller hospitals or rural areas. Additionally, surgeons require specialized training and experience to effectively use robotic systems, which can involve a steep learning curve. In some cases, robotic surgery may also involve longer setup and operating times compared to conventional methods, especially during the initial stages of adoption.
The robotic surgical system itself is composed of three main components: the surgeon console, where the surgeon sits and controls the procedure; the patient-side cart with robotic arms that hold and manipulate the surgical instruments; and a high-definition vision system that provides a magnified 3D view of the surgical area. This integration of advanced hardware and software enables seamless coordination between the surgeon’s movements and the robotic instruments.
When compared to traditional open surgery and even standard laparoscopic techniques, robotic surgery offers superior precision, better visualization, and improved overall efficiency in many cases. While laparoscopic surgery also uses small incisions, it lacks the same level of instrument articulation and depth perception provided by robotic systems. As a result, robotic surgery is particularly advantageous in complex or technically demanding procedures.
Looking toward the future, the field of robotic surgery in gynecology is expected to grow even further with continuous technological advancements. Integration with artificial intelligence may enable real-time decision support, enhanced imaging, and automated assistance during procedures. Improvements in system design could lead to more compact, affordable, and widely accessible robotic platforms. Furthermore, advancements in simulation-based training and virtual reality are likely to enhance surgical education, allowing more surgeons to develop proficiency in robotic techniques.
In conclusion, robotic surgery represents a major advancement in gynecologic care. It combines precision, innovation, and patient-centered benefits to improve surgical outcomes and overall quality of care. Although challenges such as cost and accessibility remain, ongoing developments are expected to address these issues and expand the reach of this technology. As robotic systems continue to evolve, they are poised to play an increasingly important role in shaping the future of minimally invasive gynecological surgery.